Food for Thought: The Gut Microbiome’s Impact on Mental Wellbeing
Mental wellbeing is a focus for everyone, including ourselves. Over the last two decades the gut microbiome has transitioned from a niche research topic into a credible contributor to brain function and behaviour via the gut–brain axis. The idea that gut health influences mood is not new, but modern science began confirming this in the early 2000s, when advances in microbial sequencing and animal studies revealed that gut microbes could shape behaviour and stress responses.1
The gut–brain axis in a nutshell
The gut–brain axis refers to the two-way communication network linking the gut, its resident microbiota, and the brain. This interaction involves multiple pathways, neural (via the vagus nerve), immune, hormonal, and metabolic, allowing signals from the gut to influence mood, cognition, and behaviour, and vice versa.2
- From the gut to the brain: The gut microbiota can influence brain function and mood through various mechanisms, including the production of neurotransmitters (like serotonin and gamma-aminobutyric acid), regulation of the immune system, and the release of microbial metabolites such as short-chain fatty acids that can affect brain activity and inflammation.
- From the brain to the gut: Psychological stress and emotional states can, in turn, alter gut motility, permeability, and microbial composition via neural and hormonal pathways (such as the hypothalamic–pituitary–adrenal axis).
Advances in microbiome science have shown that changes in gut microbial composition and activity can affect neurotransmitter production, inflammation, and stress responses. These discoveries have transformed how we understand mental health, highlighting that supporting the gut environment through diet and lifestyle may complement psychological or medical care.
Mental health in Australia — the picture right now
Recent national studies show mental health conditions remain a leading cause of ill health in Australia. The Australian Institute of Health and Welfare’s 2020–2022 National Study of Mental Health and Wellbeing reported that almost two in five people (38.8%) aged 16–24 years and around one in four people (26.3%) aged 25–34 years had a 12-month mental disorder.3 The Australia Burden of Disease Study (2024) also reported that mental disorders accounted for about 15% of the total burden of disease in 2024, with anxiety and depressive disorders among the largest contributors.4 These population figures matter for clinicians because prevalence and burden shape service demand, funding, and the scale of opportunity for healthcare professionals to contribute to multidisciplinary care.
Diet, the microbiome, and mental health
Our modern dietary patterns, which are often characterised by high intakes of ultra-processed foods, refined carbohydrates, and saturated fats, have not only affected physical health but also mental wellbeing. Diets low in fibre and plant diversity can lead to reduced microbial diversity and fewer beneficial metabolites such as short-chain fatty acids (SCFAs), which are known to have anti-inflammatory and neuroactive effects.5 Emerging evidence links these dietary shifts with higher risks of depression and anxiety.6
Observational and intervention studies consistently point to healthier dietary patterns being associated with lower risk or severity of depression and anxiety. The Mediterranean diet (high in vegetables, fruit, legumes, whole grains, fish, and olive oil) is the most thoroughly studied: systematic reviews and recent trials report modest but clinically relevant improvements in depressive symptoms when people adopt Mediterranean-style eating plans.7 For older adults and in several RCTs, improvements in mood and stress markers have been observed following Mediterranean diet.
Psychobiotics
The term psychobiotics was coined to describe live microorganisms (and sometimes prebiotic compounds) that when ingested produce mental health benefits via the gut–brain axis.8 One key pathway involves the gut’s pattern recognition receptors, which detect bacterial components like lipopolysaccharides (from gram-negative bacteria) and peptidoglycans (from gram-positive bacteria). When activated, these receptors can influence gut barrier function and inflammation.9
Emerging evidence also shows that gut microbes release extracellular vesicles (EVs), which are tiny packages that carry neuroactive compounds capable of affecting host signalling and potentially the brain.10 Altered gut microbiota, or dysbiosis, has been observed in conditions such as depression and autism spectrum disorder, often alongside increased gut permeability.11
Psychobiotics may work through multiple mechanisms:12
- Vagus nerve activation (direct gut–brain signalling),
- Endocrine and immune modulation, and
- Production of neuroactive metabolites that can circulate and influence the brain.
Researchers are now using advanced tools like liquid chromatography–mass spectrometry (LC–MS) to measure how these microbial compounds travel through the body, which is a crucial step toward understanding how much actually reaches the brain to impact mood and behaviour.12
Overall picture – the whole-diet approach
Emerging evidence highlights the gut microbiota as an important link between the brain, mood, and behavior, suggesting that microbiota-targeted strategies may support mental wellbeing and offer alternative therapeutic options for those unresponsive to conventional treatments.13 While specific probiotics and prebiotics (collectively termed psychobiotics) show promise, the evidence increasingly supports a whole-diet approach as the most sustainable and accessible path to improving mental wellbeing.13
Compared to supplements alone, dietary modification offers broader nutritional benefits, greater accessibility, lower cost, and the potential for synergistic effects within the gut ecosystem.13 Nutrients, fibre, and bioactive compounds from a variety of foods collectively shape microbial diversity and function, which in turn influence neurochemical and inflammatory pathways relevant to mood regulation.
One of the first studies to explore this in a healthy population was conducted by Berding et al. (2022). In this trial, participants followed a psychobiotic diet, which is rich in prebiotic- and fibre-containing foods such as whole grains, legumes, fruits, vegetables, and fermented products, for four weeks.13 Results showed a significant reduction in perceived stress, with the strongest improvements observed among participants who adhered most closely to the dietary recommendations. These findings align with a broader literature linking healthy dietary patterns, such as the Mediterranean diet, with better stress management, emotional wellbeing, and reduced risk of depression and anxiety.7,14
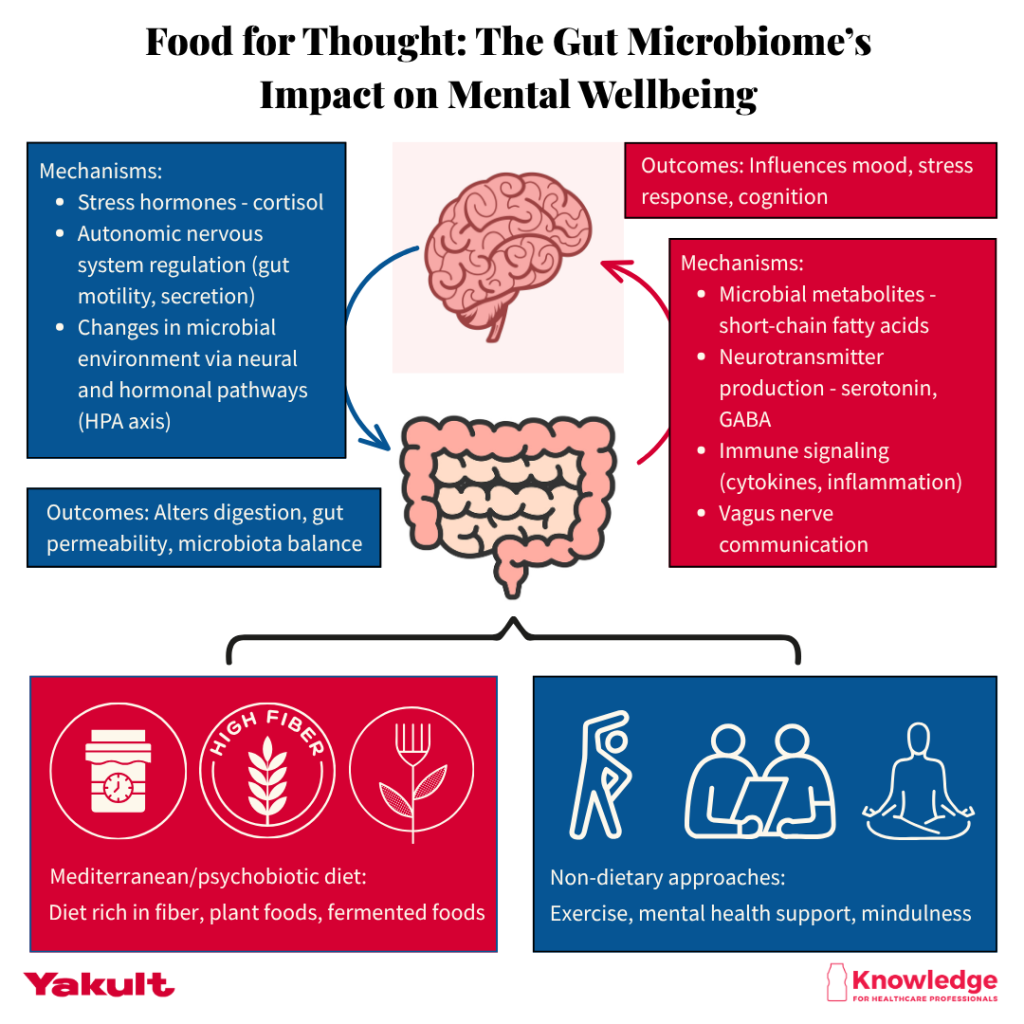
Figure 1. The bidirectional gut–brain axis. Gut microbes communicate with the brain via neural, immune, and metabolic pathways, influencing mood and stress. Brain signals also affect gut function and microbial composition. Diet and lifestyle factors help maintain a healthy, diverse microbiota to support mental wellbeing.
Conclusion
The growing body of evidence on the gut–brain axis reinforces the intricate relationship between gut health and mental wellbeing. Supporting a healthy gut microbiota through diet and lifestyle may positively influence mood, stress resilience, and overall mental health. Whole-diet approaches rich in fibre, plant foods, and fermented products appear particularly promising for maintaining a diverse and stable gut environment, which is a key foundation for both physical and mental health.
Incorporating fermented foods, such as those containing probiotic bacteria like Lacticaseibacillus paracasei Shirota (LcS) found in Yakult, could be one practical way to help maintain gut health as part of a balanced diet. However, mental health is multifactorial, and optimal wellbeing depends on more than nutrition alone. Non-dietary strategies such as regular physical activity, quality sleep, and stress-management practices complement dietary interventions and play equally important roles in supporting overall mental health.
Take-home messages:
- The gut–brain axis connects the gut microbiota and the central nervous system through neural, immune, and metabolic pathways.
- Gut health plays an integral role in regulating stress and mood.
- Diets low in fibre and high in ultra-processed foods, can reduce microbial diversity and potentially affect mental wellbeing.
- Dietary patterns rich in plant-based foods, whole grains, legumes, nuts, and fermented foods, such as those featured in the Mediterranean and psychobiotic diets, may support a healthy microbiota and reduce perceived stress.
- Non-dietary lifestyle factors, including regular exercise, adequate sleep, stress-reduction practices, and social support, are essential companions to dietary change in improving mental health outcomes.
- Encouraging clients to focus on overall dietary quality, alongside mental health support, can offer a holistic approach to wellbeing.
References:
- Lewandowska-Pietruszka Z, Figlerowicz M, Mazur-Melewska K. The History of the Intestinal Microbiota and the Gut-Brain Axis. Pathogens. 2022; 11(12). Doi: 10.3390/pathogens11121540
- Mayer EA, Tillisch K, Gupta A. Gut/brain axis and the microbiota. J Clin Invest. 2015 Mar 2;125(3):926-38. doi: 10.1172/JCI76304.
- Australian Bureau of Statistics. National survey of mental health and wellbeing. Australian Bureau of Statistics. Published October 5, 2023. https://www.abs.gov.au/statistics/health/mental-health/national-study-mental-health-and-wellbeing/latest-release
- Mental Health. Mental illness burden of disease. Australian Institute of Health and Welfare. Updated August 19, 2025. https://www.aihw.gov.au/mental-health/topic-areas/health-wellbeing/burden-of-disease
- Bindels LB, Delzenne NM, Cani PD, Walter J. Towards a more comprehensive concept for prebiotics. Nat Rev Gastroenterol Hepatol. 2015;12:303. doi: 10. 10.1038/nrgastro.2015.47
- Lee M, Bradbury J, Yoxall J, Sargeant S. Is dietary quality associated with depression? An analysis of the Australian longitudinal study of women’s health data. Br J Nutr. 2022;129(8):1-8. doi: 10.1017/S0007114522002410.
- Altun A, Brown H, Szoeke C, Goodwill AM. The Mediterranean dietary pattern and depression risk: A systematic review. Neurol Psychiatry Brain Res. 2019; 33:1-10. doi: 10.1016/j.npbr.2019.05.007
- Cryan JF, Dinan TG. Mind-altering microorganisms: The impact of the gut microbiota on brain and behaviour. Nature Reviews. Neuroscience. 2012;13 (10):701–12. doi: 10.1038/nrn3346.
- Montagnani M, Bottalico L, Maria Assunta Potenza, et al. The Crosstalk between Gut Microbiota and Nervous System: A Bidirectional Interaction between Microorganisms and Metabolome. 2023;24(12):10322-10322. doi:https://doi.org/10.3390/ijms241210322
- Molina-Tijeras JA, Gálvez J, Rodríguez-Cabezas ME. The Immunomodulatory Properties of Extracellular Vesicles Derived from Probiotics: A Novel Approach for the Management of Gastrointestinal Diseases. Nutrients. 2019;11(5):1038. doi:https://doi.org/10.3390/nu11051038
- Teskey G, Anagnostou E, Mankad D, et al. Intestinal permeability correlates with behavioural severity in very young children with ASD: A preliminary study. Journal of Neuroimmunology. 2021; 357:577607. doi: https://doi.org/10.1016/j.jneuroim.2021.577607
- Kyei-Baffour VO, Akshay Kumar Vijaya, Aurelijus Burokas, Daliri EBM. Psychobiotics and the gut-brain axis: advances in metabolite quantification and their implications for mental health. Critical Reviews in Food Science and Nutrition. Published online February 5, 2025:1-20. doi:https://doi.org/10.1080/10408398.2025.2459341
- Berding K, Bastiaanssen TFS, Moloney GM, et al. Feed your microbes to deal with stress: a psychobiotic diet impacts microbial stability and perceived stress in a healthy adult population. Molecular Psychiatry. 2022;28. doi:https://doi.org/10.1038/s41380-022-01817-y
- Molendijik M, Molero P, Sánchez-Pedreño FO, Van der Does W, Martínez-González MA. Diet quality and depression risk: A systematic review and dose-response meta-analysis of prospective studies. J Affect Disord. 2018: 226: 346-354. doi:10.1016/j.jad.2017.09.022
- Loughman A, Staudacher HM. How can I improve my gut health via non-dietary means? Lancet Gastroenterol Hepatol. 2024 Jan;9(1):20. doi: 10.1016/S2468-1253(23)00412-0.
